Prostate Cancer
Abnormal enlargement of the prostate, a condition called hyperplasia of the prostate or benign enlargement of the prostate, is common among men fifty years and older. As the enlarged prostate can press on the urethra. Such pressures can hinder the passage of urine and may result in bladder infection or kidney damage. In many cases, treatment includes the surgical removal of part or the entire prostate.
Cancer of the prostate can also strike older men. In most cases, it spreads to other parts of the body before being detected. All prostate tissues, be it normal, hyperplastic and cancerous, are stimulated by the male hormone testosterone, which is produced by the testicles. If the cancer has spread widely, physicians treat it with female hormones or by castration, which is removal of the testicles surgically. If the cancer has not spread beyond the prostate, the diseased tissue is removed.
Adenocarcinoma is the term used to identify cancer of gland cells.The genetic changes which occur in cancer include the mutation of key regulatory genes, changes in protein products and changes in the amount of product produced by genes, which arereferred to as gene expression. As changes accumulate cells become more abnormal causing cancer to progress.
Some of the genes that have been shown to be important in the development of prostate cancer are:
The Androgen Receptor
Androgens are male hormones. One such example is testosterone. These receptors are proteins which can be found within the cell that help control growth and division. Once an androgen enters the cell and binds toandrogen receptors, the complex acts as a transcription factor, promoting cell growth. These receptors are important regulators of normal cell growth in the prostate, (Emory University, 2013).
PTEN Gene
PTEN, refers to phosphatase and tensin, homolog deleted on chromosome 10 is a tumor suppressor gene of which has often mutated in prostate cancer. This gene plays an important role in several cellular pathways, including the control of prostate basal cell growth. Mouse models suggest that by the proliferation of these cells early progression of prostate cancer may be evident, (Emory University, 2013).
P53 Gene
P53 which is a tumor suppressor gene involved in DNA repair and the regulation of apoptosis, also causes mutations in a small fraction of prostate cancers and are usually associated with metastatictumors, (Emory University, 2013).
Cancer of the prostate can also strike older men. In most cases, it spreads to other parts of the body before being detected. All prostate tissues, be it normal, hyperplastic and cancerous, are stimulated by the male hormone testosterone, which is produced by the testicles. If the cancer has spread widely, physicians treat it with female hormones or by castration, which is removal of the testicles surgically. If the cancer has not spread beyond the prostate, the diseased tissue is removed.
Adenocarcinoma is the term used to identify cancer of gland cells.The genetic changes which occur in cancer include the mutation of key regulatory genes, changes in protein products and changes in the amount of product produced by genes, which arereferred to as gene expression. As changes accumulate cells become more abnormal causing cancer to progress.
Some of the genes that have been shown to be important in the development of prostate cancer are:
The Androgen Receptor
Androgens are male hormones. One such example is testosterone. These receptors are proteins which can be found within the cell that help control growth and division. Once an androgen enters the cell and binds toandrogen receptors, the complex acts as a transcription factor, promoting cell growth. These receptors are important regulators of normal cell growth in the prostate, (Emory University, 2013).
PTEN Gene
PTEN, refers to phosphatase and tensin, homolog deleted on chromosome 10 is a tumor suppressor gene of which has often mutated in prostate cancer. This gene plays an important role in several cellular pathways, including the control of prostate basal cell growth. Mouse models suggest that by the proliferation of these cells early progression of prostate cancer may be evident, (Emory University, 2013).
P53 Gene
P53 which is a tumor suppressor gene involved in DNA repair and the regulation of apoptosis, also causes mutations in a small fraction of prostate cancers and are usually associated with metastatictumors, (Emory University, 2013).
Risk Factors of Prostate Cancer
- Age: The risk of prostate cancer increases dramatically with age. In most cases,patients are diagnosed with the disease over the age of fifty.
- Family history: It is possible to inherit dysfunctional genes that lead to the development of a familial form of a particular cancer type. Individuals with a family history of prostate cancer are therefore at an increased risk of developing the disease.
- Race: Prostate cancer has shown to affect a greater number of African men world-wide.
- Dietary Factors: Studies indicate that many dietary factors may influence prostate cancer risk. It has been suggested that a diet rich in dairy and meat products may be associated with ahigher risk, while a diet rich in fish and tomato - based products may be associated with lower risk of prostate cancer.
Signs and Symptoms
Currently, most cases of prostate cancer are identified by screening in asymptomatic men. However, most cases of prostate cancer are diagnosed before symptoms develop through screening. According to the American Cancer Society, symptoms associated with later-staged prostate cancer includes inability to urinate, discontinuous or weak urine flow, difficulty in starting or stopping urine flow, frequent urination, especially at night, blood in urine, pain or burning with urination and continuous back, pelvis, or upper thigh pain. It is important to note, that these symptoms may be from diseases other than prostate cancer,therefore physical examination alone cannot reliably differentiate benign prostatic disease from cancer, (American Cancer Society, 2013).
Currently, most cases of prostate cancer are identified by screening in asymptomatic men. However, most cases of prostate cancer are diagnosed before symptoms develop through screening. According to the American Cancer Society, symptoms associated with later-staged prostate cancer includes inability to urinate, discontinuous or weak urine flow, difficulty in starting or stopping urine flow, frequent urination, especially at night, blood in urine, pain or burning with urination and continuous back, pelvis, or upper thigh pain. It is important to note, that these symptoms may be from diseases other than prostate cancer,therefore physical examination alone cannot reliably differentiate benign prostatic disease from cancer, (American Cancer Society, 2013).
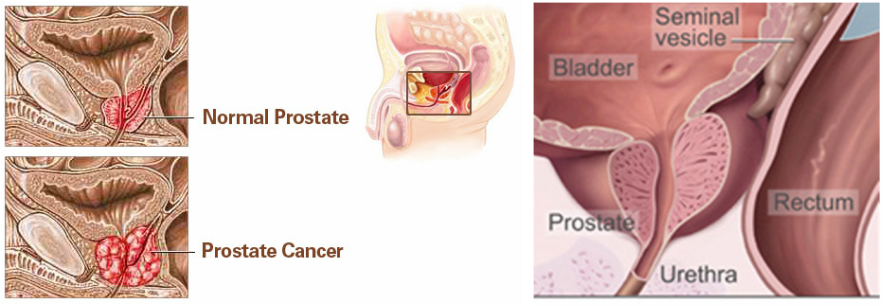
Pictures of Normal Prostate and Prostate Cancer
Detection and Diagnosis of Prostate Cancer
Only a doctor can diagnose cancer. However, in many cases, a doctor is only consulted after the disease is far advanced. A person should therefore be alert to any physical changes that may be a symptom of cancer. Early detection greatly increases the chances of a cure.
Cancer shows no symptoms in its beginning stages but symptoms may appear before the disease spreads. The American Cancer society lists seven such warning signals. They include changes in the bowel or bladder habits, a sore that does not heal, unusual bleeding or discharge, thickening or lump in testicles, indigestion or difficulty swallowing, obvious change in wart or mole and nagging cough or hoarseness. (2013 American Cancer Society)
Prostate cancer is detected in several ways. These include screening, digital rectal examinations, prostate specific antigen, also referred to as PSA test and biopsy. The method used depends, in part, on the patient's preference and whether the cancer is causing any symptoms.
Screening
The American Cancer Society recommends that men decide whether to be screened for prostate cancer based on a discussion with their health care provider about the uncertainties, risks, and potential benefits of screening, (American Cancer Society, 2013)
The recommended age for starting screening is fifty years of age for men at average risk who have at least a ten-year life expectancy, forty or forty-five years of age for African Americans and men who have had a first-degree relative diagnosed with prostate cancer before age sixty-five years and forty years of age for men with several first-degree relatives who had prostate cancer at an early age.
Digital Rectal Exams
Digital rectal exams are very useful for the detection of abnormalities, including cancer, in the rectum. A doctor inserts a gloved, lubricated finger in the rectum and feels for abnormalities. In men, digital rectal exams are also used to detect changes in prostate that could indicate an abnormal condition, including cancer. The procedure is very quick and although it may be uncomfortable, it is not painful, (World Book, 1997).
Prostate Specific Antigen (PSA)
The prostate specific antigen is a glycoprotein produced by prostate cells and is a normal component of semen. In general, a PSA level less than 4 ng/ml is considered normal and greater than 10 ng/ml is considered high. Levels between 4 and 10 ng/ml represent a grey area in which a doctor may consider a digital rectal exam before recommending further testing. When abnormal events occur in the prostate, such as prostate cancer, the overabundance of prostate cells, the overproduction of PSA, or the leaking of PSA into the bloodstream may result in a measurable increase in the level of PSA in the blood. Blood tests are used to assess the level of PSA in the blood. A level higher than normal of PSA might indicate a problem with the prostate, however is not limited to cancer, (American Cancer Society, 2013)
Biopsy
Non-invasive diagnostic techniques, like Magnetic Resonance Imaging (MRI), Ultrasound, Computed Tomography (CT) scan or Positron Emission Tomography (PET) scan, are very useful but in some cases when a suspicious abnormality or lesion is discovered a doctor may perform a biopsy to determine its exact characteristics. A biopsy is the removal of either a portion of a lesion incisional or the entire lesion excisional. The tissue is then sent to a lab where a pathologist will diagnose the sample, (Emory University, 2013).
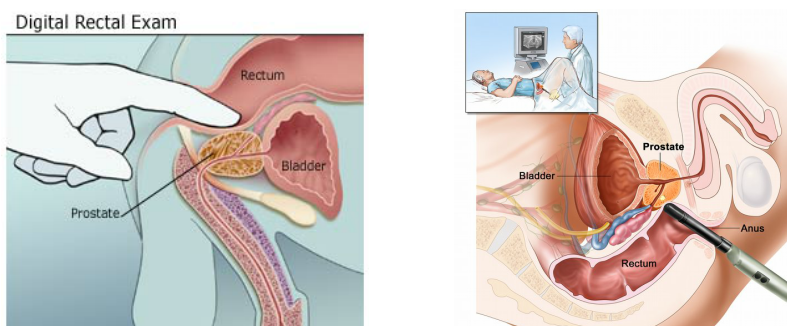
Picture of A Digital Rectal Examination Picture of A Doctor doing an Ultrasound of Prostate
Treatment of Prostate Cancer
The treatment of prostate cancer can be broken down into two categories: early stage and advanced stage. Early stage treatment involves tumors that are confined to the prostate. Advanced stage treatment involves tumors that have spread beyond the prostate gland. Treatment options are dependent upon size of tumor, location, physical condition of patient, and stage of cancer.
The National Comprehensive Cancer Network (NCCN) lists the following treatments for prostate cancer watchful waiting, radical prostatectomy, transurethral resection of the prostate (TURP), external beam radiation, internal radiation, hormone therapy, removal of the testicles known as orchiectomy, antiandrogens and chemotherapy.
References:
WebMD. (2005). Retrieved from Prostate Cancer Health Center: http://www.webmd.com/prostate-cancer/default.htm
Macmillian. (2012, 05 01). Retrieved from Cancer Support: http://www.macmillan.org.uk/Cancerinformation/Cancertypes/Prostate/Prostatecancer.aspx
Publishers, K. A. (1995, 05 01). Springer Link. Prostate gland: Structure, functions and regulation, 231-243. Retrieved from Prostate gland: Structure, functions and regulation: http://link.springer.com/article/10.1007%2FBF02564756
WebMD. (2005). Retrieved from Prostate Cancer Health Center: http://www.webmd.com/prostate-cancer/default.htm
Macmillian. (2012, 05 01). Retrieved from Cancer Support: http://www.macmillan.org.uk/Cancerinformation/Cancertypes/Prostate/Prostatecancer.aspx
Publishers, K. A. (1995, 05 01). Springer Link. Prostate gland: Structure, functions and regulation, 231-243. Retrieved from Prostate gland: Structure, functions and regulation: http://link.springer.com/article/10.1007%2FBF02564756